
Peruzzi P, Bergese SD, Viloria A, et al.Awake craniotomy for brain tumor resection: the rule rather than the exception? J Neurosurg Anesthesiol. 
Awake craniotomy vs surgery under general anesthesia for resection of supratentorial lesions. Sacko O, Lauwers-Cances V, Brauge D, et al.Functional outcome after language mapping for insular World Health Organization Grade II gliomas in the dominant hemisphere: experience with 24 patients. Duffau H, Moritz-Gasser S, Gatignol P.Awake mapping optimizes the extent of resection for low-grade gliomas in eloquent areas. De Benedictis A, Moritz-Gasser S, Duffau H.Cortical mapping and local anaesthetic resection as an aid to surgery of low and intermediate grade gliomas. Cortical mapping for defining the limits of tumor resection. Intraoperative brain mapping techniques in neuro-oncology. The feasible synergy between image-guided stereotactic surgery and awake craniotomies has resulted in the desired outcome of safe maximum resection in patients with malignant tumors within eloquent regions of the brain. Moreover, more than 80% are discharged on the first postoperative day. Overall, patients report adequate pain control and universal satisfaction with comfort during surgery. On average, we perform four to five awake craniotomies monthly for primary brain tumors and brain metastases, as well as for symptomatic steroid-refractory radiation necrosis adjacent to eloquent cortex. Patients receive educational information regarding what the procedure entails and potential expectations. The program is largely a collaborative effort between neurosurgical oncology, anesthesia, clinical neuropsychology, and neurophysiology. The scalp blocks with long-acting local anesthetics do provide reasonable intraoperative and postoperative pain control.11 The reduced need for postoperative intravenous narcotics with awake craniotomy minimizes the likelihood of narcotic- related side effects.Īt our cancer center, we have an established awake-craniotomy program for tumors in eloquent cortex. 9,10 Incorporation of intermittent sedation can be very valuable as well. Studies assessing the subjective experiences of patients during awake craniotomy for the most part demonstrate reasonable tolerance for the procedure. Patient comfort during surgery, especially with respect to minimizing fatigue, is always a critical component of awake craniotomy, since patient cooperation is vital to the surgical outcome. A malignant glioma with associated white matter fibers involving the left temporal lobe in a patient with speech symptoms, thus a candidate for an awake craniotomy for tumor resection. A malignant glioma with associated corticospinal motor fibers involving the motor cortex area of the left frontal lobe, hence a candidate for an awake craniotomy for tumor resection. 7 Shorter hospital stays realized with awake craniotomy translate into decreased hospital expenses. A recent review of 951 patients, some of whom underwent awake craniotomy (n = 411) and others standard craniotomy (n = 540), documented much shorter hospital stays and quick functional recovery within the group treated with awake craniotomy. 4,6 The availability of intraoperative mapping and functional delineation provides reasonable confidence with tumor resection.Īwake craniotomy has additional advantages over standard craniotomy with general anesthesia. 4-6 Awake craniotomies undoubtedly achieve superior extent of resection in eloquent regions when compared to standard craniotomies that employ general anesthesia for similar lesions. 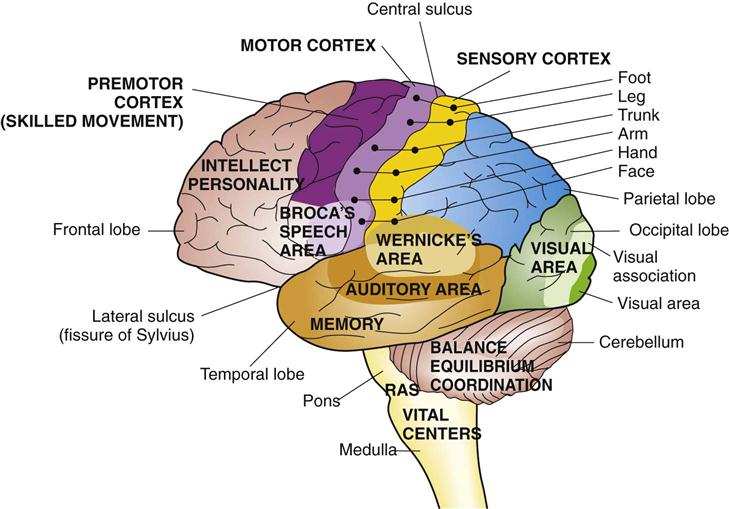
Accordingly, awake craniotomies are often associated with great functional outcomes. 
Similarly, patients are tested functionally during tumor resection, which is often terminated if at any point the patient develops deficits related to the area of eloquence. 1-3 Hence, activation of motor activity or disruption of speech during electrical stimulation strongly suggests that the stimulated area is critical and necessary for functional preservation. Local anesthesia in the form of a scalp block with mild intermittent sedation is often sufficient.ĭuring the operation, intraoperative mapping is often performed and remains the gold standard for delineation of the relationship of tumor to eloquent cortex. Patients are typically conscious during most of the procedure, which is often carried out in the absence of general anesthesia. Awake craniotomies are traditionally reserved for, but not limited to, tumors involving the primary motor ( Figure 1) and speech ( Figure 2) areas.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
